Fungal nail infections are extremely common — it’s estimated that around 3% of the UK population has one at any given time. Despite this, they’re often left untreated for years because people assume nothing can be done, or because the treatments they’ve tried haven’t worked.
The truth is that fungal nail infections do respond to treatment — but they require patience, consistency and, in many cases, guidance from a podiatrist to clear effectively.
What is a fungal nail infection?
A fungal nail infection — known medically as onychomycosis — occurs when fungi invade the nail or the skin beneath it. The same group of fungi that cause athlete’s foot (dermatophytes) are responsible for most nail infections, though yeasts and moulds can also cause them.
The toenails are far more commonly affected than fingernails, particularly the big toenail, because the feet provide the warm, moist environment fungi thrive in.
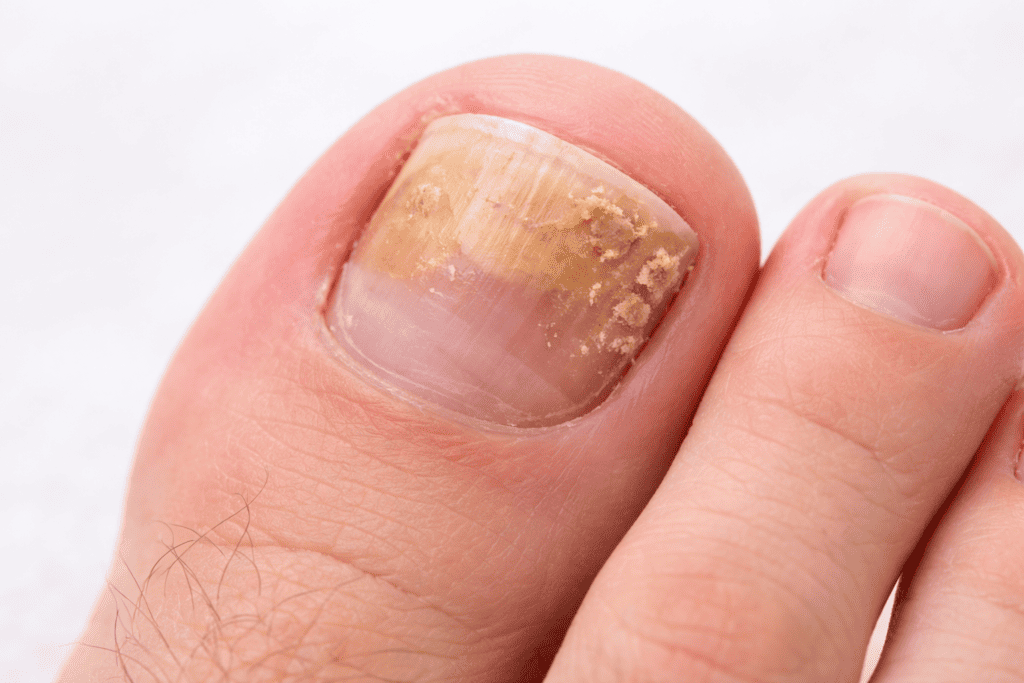
What does a fungal nail infection look like?
Fungal nail infections typically develop gradually. Early signs include:
- A white or yellow spot at the tip of the nail or under the nail edge
- The nail beginning to thicken
- A slight change in colour — yellowing, browning or whitening
As the infection progresses, the nail may:
- Become significantly thickened and difficult to cut
- Turn yellow, brown, white or even greenish
- Become crumbly or brittle, breaking away at the edges
- Separate from the nail bed (a condition called onycholysis)
- Develop a slightly unpleasant smell
- Cause mild discomfort, particularly when wearing shoes
In severe cases the entire nail may be affected and become distorted in shape.
What causes fungal nail infections?
Fungi are present in the environment around us all the time. A nail infection develops when conditions allow them to take hold and multiply. Common causes and risk factors include:
Athlete’s foot — the most common route. Athlete’s foot (tinea pedis) is a fungal skin infection that frequently spreads to the nails if left untreated. If you have recurring athlete’s foot, treating it promptly reduces the risk of nail involvement.
Communal areas — walking barefoot in swimming pool changing rooms, gym showers and communal bathing areas exposes feet to fungi.
Trauma to the nail — injury to a nail creates an entry point for fungi. Runners and people who participate in sports that put repeated stress on the toenails are particularly vulnerable.
Footwear — tight shoes that press the toes together, or non-breathable synthetic footwear that keeps the foot warm and sweaty, creates ideal conditions for fungal growth.
Age — fungal nail infections become more common with age. Older nails grow more slowly and may develop small cracks that provide entry points for fungi.
Health conditions — diabetes, poor circulation, a weakened immune system and psoriasis all increase the risk of developing a fungal nail infection and can make it harder to treat.
How is a fungal nail infection diagnosed?
Many people self-diagnose based on the appearance of their nail — and in straightforward cases they’re often right. However, several other conditions can cause similar changes to the nail, including psoriasis, nail trauma, and certain skin conditions. Treating a non-fungal nail problem with antifungal medication is ineffective and delays proper treatment.
If there’s any doubt, a podiatrist can take a nail clipping or scraping and send it for laboratory analysis to confirm the presence of fungi before recommending treatment. This is particularly worthwhile before starting a prolonged course of oral antifungal medication.
Over-the-counter treatments
For mild infections — where less than half the nail is affected and the nail root is not involved — over-the-counter antifungal treatments are a reasonable starting point.
Antifungal nail lacquers and paints
Products containing amorolfine (such as Curanail or Loceryl) or ciclopirox are applied directly to the nail like a nail varnish. They penetrate the nail and deliver antifungal medication to the infected tissue.
For these to work you need to:
- File the nail surface before each application to help the lacquer penetrate
- Apply consistently — weekly for amorolfine, daily for ciclopirox
- Continue treatment for 6 to 12 months — the full time it takes for a toenail to grow out
- Keep the feet clean and dry throughout
The most common reason these treatments fail is stopping too early. The nail may look better after a few months, but the infection is not cleared until a completely healthy nail has grown through to the tip.
Antifungal nail solutions
Products such as Nailner work by creating an environment hostile to fungi rather than delivering medication into the nail. They are generally considered less effective than lacquers for established infections but can be useful for very early or mild cases.
Prescription treatments
For moderate to severe infections — where more than half the nail is affected, multiple nails are involved, or the nail root is affected — prescription treatments are usually needed.
Oral antifungal tablets
Terbinafine tablets are the most effective treatment for toenail fungal infections, with cure rates of around 70 to 80% when taken as prescribed. Treatment typically lasts 3 months for toenails.
Terbinafine is generally well tolerated but is not suitable for everyone. Your GP will check for any drug interactions and may want to monitor liver function during treatment. It is not recommended during pregnancy.
Ask your GP for a referral or visit a podiatrist who can advise on whether oral treatment is appropriate for you.
Professional podiatry treatments
Nail debridement
A podiatrist can mechanically reduce a thickened, infected nail — filing it down and removing infected material. This doesn’t cure the infection on its own, but it makes topical treatments more effective by reducing the amount of infected nail tissue and improving penetration of antifungal medication. It also makes the nail more comfortable and easier to manage.
Lunula laser therapy
Lunula laser is a cold laser treatment that works by delivering two wavelengths of laser light to the nail and surrounding tissue. One wavelength targets the fungi directly; the other stimulates the immune response in the surrounding tissue.
Unlike some other laser devices used for nail infections, Lunula is cold and painless — there is no heat sensation. Clinical evidence shows good results, particularly when combined with topical antifungal treatment. A typical course consists of 4 treatments over 4 weeks.
PACT photodynamic therapy
PACT (Photodynamic Antimicrobial Therapy) involves applying a photosensitising gel to the nail and then activating it with a specific wavelength of light. This generates a reaction that destroys the fungal cells. It is painless and has no systemic side effects — making it a good option for people who cannot take oral medication.
How long does treatment take?
This is the most important thing to understand about fungal nail infections: treatment takes time because nails grow slowly. Even if the treatment kills the fungi quickly, you won’t see a fully clear nail until a healthy nail has grown through from the root to the tip — which takes 9 to 18 months for toenails.
Progress can be monitored by marking the base of the nail where healthy growth begins and watching that clear area extend toward the tip over time.
Preventing fungal nail infections
- Treat athlete’s foot promptly — don’t let it spread to the nails
- Wear flip-flops in communal changing rooms and pool areas
- Keep feet clean and dry, particularly between the toes
- Wear breathable footwear and moisture-wicking socks
- Don’t share towels, nail clippers or files
- Trim nails straight across and not too short
- If you use a nail salon, make sure they sterilise instruments between clients
When should you see a podiatrist?
- More than half the nail is affected
- Multiple nails are involved
- Over-the-counter treatment hasn’t improved things after 3 months
- You have diabetes, poor circulation or a weakened immune system
- The nail is causing pain or making it difficult to walk
- You’re not sure whether it’s a fungal infection
Find a podiatrist near you
A podiatrist can confirm your diagnosis, reduce a thickened nail and advise on the most effective treatment for your situation — including laser therapy where available. Search our directory to find HCPC-registered specialists near you.
This article is for general information only and does not constitute medical advice. Always consult a qualified, HCPC-registered practitioner for diagnosis and treatment of any foot condition.
Written by
FootcareUK Editorial Team
Our articles are written and reviewed by qualified foot health professionals including podiatrists and chiropodists. The FootcareUK editorial team is committed to providing accurate, up-to-date information to help you make informed decisions about your foot health care.